OVERVIEW
The UCSF Ophthalmology research curriculum is designed to give residents the epidemiological and biostatistical tools that they need to become productive members of the research community. Over the year-long course, residents will receive instruction in study design, parametric and non-parametric statistical methodology, and data presentation. In addition, residents will receive instruction in R programming. These lectures are incorporated into the instructional curriculum for the UCSF Ophthalmology Residency program, and occur on Thursday of every week during the academic year, which runs from September to June.
The capstone project of the curriculum is the performing a clinical, translational or basic science resident research project. Residents will progress from project conception to design to completion with the help from a faculty mentor. These projects are presented as part of the annual Alexander Irvine Resident’s Day each May.
SCHEDULE
July
Residents meet with potential mentors, determine area of interest
Research Workshop Day – an all-day lecture series on the basics of study design and introduction to statistics.
August
Residents develop research proposals
Meet with faculty epidemiologist, Dr. Ben Arnold
Residents present project proposals to a panel of faculty and the department chairperson.
September to December
Epidemiology lecture series (see resident lecture schedule)
R programming modules (see resident lecture schedule for assignments)
Perform research projects
December
Mid-year project review with Dr. Arnold and Dr. Schallhorn
January to April
Epidemiology lecture series
R programming modules
Perform research projects
May
Alexander Irvine Residents Day
READINGS
Residents are required to read the Lancet epidemiology series, available on the UCSF Ophthalmology Residency Box site.
Residents conducting clinical trials are required to read Designing Clinical Research by Stephen B. Hulley, MD, MPH et al. Wolters Kluwer. 4th Edition. 2013. UCSF library call number: R853.C55 D47
FACULTY MENTOR
The resident research curriculum is overseen by Dr. Julie Schallhorn, Associate Residency Program Director. Dr. Benjamin Arnold provides epidemiology mentorship. All residents are asked to select an additional faculty member who is specialized in their area of research interest
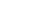

 The UCSF-Proctor Clinician Vision Scholars K12 Program is a $2.5 million, five-year grant from the National Eye Institute (NEI), one of 27 institutes and centers that comprise the US National Institutes of Health. This grant provides institutional funding to train as many as ten young faculty members to achieve this same level of success. Co-led by Yvonne Ou, MD, and Tom Lietman, MD – both NEI grant awardees – the program builds on existing strengths and collaborations in clinical and translational sciences, bioengineering, and career development in the UCSF Proctor Foundation and Department of Ophthalmology.
The UCSF-Proctor Clinician Vision Scholars K12 Program is a $2.5 million, five-year grant from the National Eye Institute (NEI), one of 27 institutes and centers that comprise the US National Institutes of Health. This grant provides institutional funding to train as many as ten young faculty members to achieve this same level of success. Co-led by Yvonne Ou, MD, and Tom Lietman, MD – both NEI grant awardees – the program builds on existing strengths and collaborations in clinical and translational sciences, bioengineering, and career development in the UCSF Proctor Foundation and Department of Ophthalmology.