Dr. Seth Blumberg, MD, joins UCSF’s Francis I. Proctor Foundation as a computational epidemiologist. He provides patient care to hospitalized patients at UCSF Medical Center as an internist specializing in infectious disease.
Fellowships: New York University (infectious diseases), Proctor Foundation (forecasting trachoma control), National Institutes of Health (research and policy for infectious disease dynamics)
Residency: St. Mary’s Medical Center, San Francisco
MD, PhD: University of Michigan, Ann Arbor (PhD in Biophysics)
 How did Hodgkin’s disease shape your career? I was a classic “Caltech nerd,” pursuing math and physics, when I was diagnosed with cancer. Fortunately, my treatment was effective, and I got a second chance at life. Becoming a clinician and medical researcher became my way of giving back.
How did Hodgkin’s disease shape your career? I was a classic “Caltech nerd,” pursuing math and physics, when I was diagnosed with cancer. Fortunately, my treatment was effective, and I got a second chance at life. Becoming a clinician and medical researcher became my way of giving back.
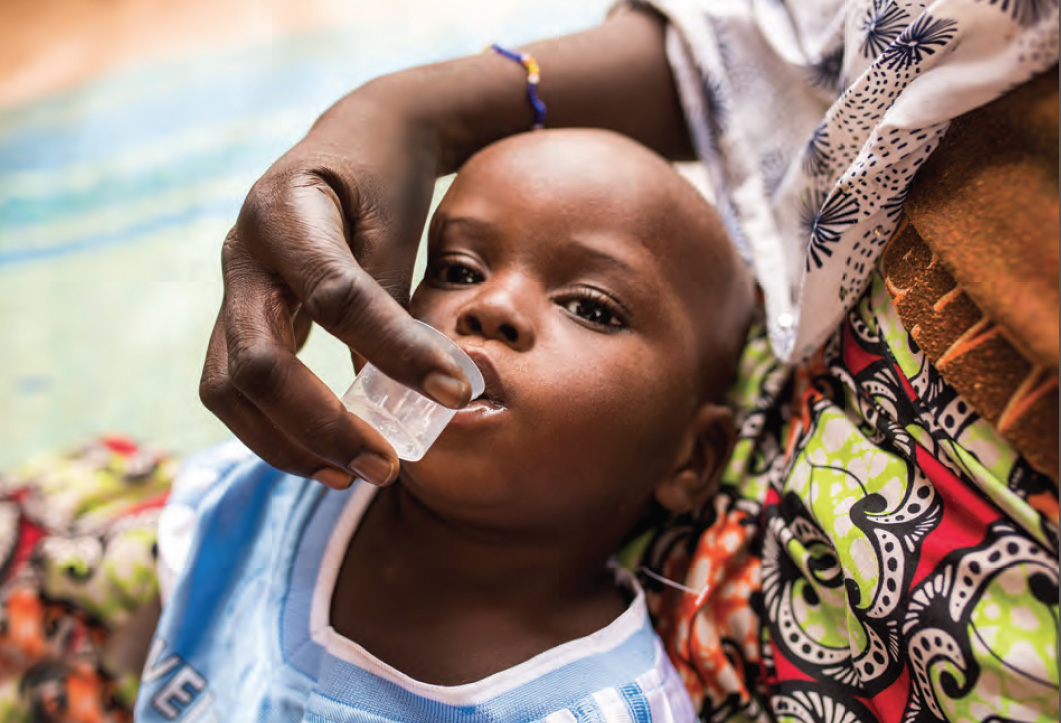
How do your skills strengthen the Proctor Foundation’s capacity to improve public health and protect sight? My training and experience in mathematical modeling, infectious disease dynamics, and biophysics complements rich existing knowledge and skills. An interdisciplinary approach allows our research team to tackle complex public health questions to address ongoing spread of preventable diseases, including blindness caused by trachoma.
How is Proctor providing leadership on the threat of antimicrobial-resistant infections? The Centers for Disease Control (CDC) funds our investigation of antimicrobial resistance in the United States. Ironically, the antibiotics we use to treat serious infections can also increase the risk of deadly infections from Newsresistant bacteria. Our research aims to figure out how to treat infections without unintended consequences. We hope to build on this research and study patterns of resistance in low- and middle-income nations.
How has COVID-19 altered your research? In June 2020, the CDC reached out to Proctor, requesting that we immediately begin analyzing COVID data from US hospitals to help decrease transmission and improve outcomes. To reduce the rapid spread inside California prisons, I volunteered as an epidemiological modeler with AMEND, a university-based prison health consortium.
What did you gain in your RAPIDD Fellowship at the National Institutes of Health Fogarty Center? RAPIDD stands for Research and Policy for Infectious Disease Dynamics. I collaborated with outstanding leaders who advanced the field of mathematical modeling of epidemiologic data to understand, forecast, and mitigate the transmission potential of emerging diseases. This methodology helps guide governmental and international health policy – to manage novel disease threats and save lives.